NHS trusts across England could be spending more than £13.5 million each year correcting data problems that emerge after Electronic Patient Record (EPR) transitions.
An EPR transition is the changeover from a legacy hospital system or an existing EPR to a new one, involving the movement of patient data, clinical workflows, and operational processes to a new digital platform.
These programmes are central to modernising the NHS and improving coordination between services – but they also expose a problem that is often underestimated. Without undertaking the necessary data due diligence, hidden inconsistencies in legacy data – including duplicate pathways, missing outcomes, and incomplete records – often only become visible once the new system goes live. At that point, they begin to affect how organisations track patients, manage waiting lists, and report performance.
Where the problem becomes visible: waiting lists
The impact is most clearly seen in Patient Tracking Lists (PTLs). MBI’s analysis suggests that PTLs increase by around 25% on average following an EPR go-live. This is not a reflection of new demand, but of inaccuracies exposed or introduced during transition, such as duplicated pathways appearing in multiple places.
Because PTLs underpin Referral to Treatment (RTT) performance – the primary measure of elective recovery – instability here makes it harder for trusts to understand who is waiting. This impacts their ability to prioritise patients safely and maintain control of performance. For many organisations, this period of instability lasts four to six months whilst teams work to stabilise reporting and rebuild confidence in the data, hindering efforts to meet targets in line with key government priorities.
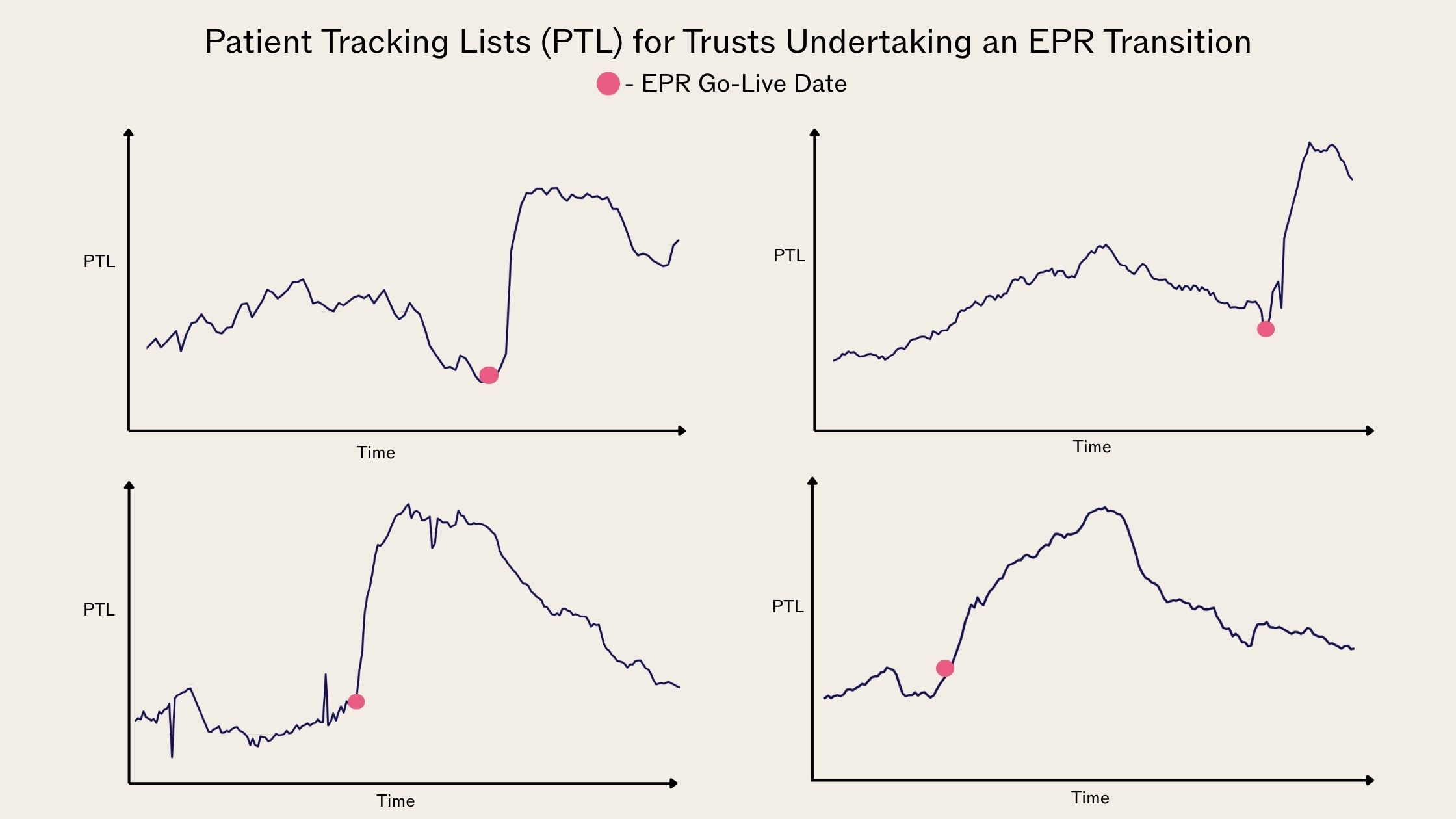
Why issues emerge after go-live
Legacy data frequently contains inconsistencies – missing clinical outcomes, duplicate pathways, incorrect clock positions, or events recorded in documents that don’t have a suitable place in the structure of the new system. These issues may sit within legacy systems for years without causing visible disruption, as local teams develop workarounds to manage them.
However, a transition changes that environment – data is reinterpreted through new rules and reporting structures. At that point, inconsistencies that were previously tolerated begin to affect operational control. This follows a consistent pattern: risks remain hidden before go-live, surface during migration, and then appear afterwards as instability in reporting and increased reliance on manual validation. This is why post-go-live disruption is often misattributed. What appears to be a problem with the new EPR system is frequently a consequence of legacy data that has not been fully understood or prepared before transition.
The wider operational and patient impact
The £13.5 million estimate captures only the direct cost of correcting data once systems are live. The broader impact is operational. When organisations lose confidence in their PTL, staff time is diverted from patient care to checking records, affecting clinical decision-making and patient progression. Reporting cycles become more complex, and performance management less certain. This has a direct effect on productivity, and how care is delivered.
There are also implications for patient safety. A review by the Health Services Safety Investigations Body (HSSIB) has linked EPR transitions to incidents where care was missed, delayed or incorrect, in some cases leading to significant patient harm.
London North West: stabilisation after go-live
London North West University Healthcare NHS Trust provides a clear example of how these issues present in practice, and what recovery can require. Following the implementation of Oracle Cerner Millennium in July 2023, the Trust experienced a rise in RTT pathways over the following six months, alongside a range of data quality issues that reduced confidence in the PTL and increased pressure during reporting cycles.
Working with MBI, the Trust undertook a comprehensive manual validation programme to correct pathways, reduce inconsistencies and re-establish a reliable view of the elective backlog. Removal rates reached up to 70%, allowing the PTL to return to a position that supported confident reporting and day-to-day operational decision-making.
What followed is equally important. Once stability had been restored, the Trust focused on building resilience. Automation through ROVA° was introduced into an established validation rhythm and aligned with the Federated Data Platform, ensuring that it strengthened existing governance processes rather than replacing them. The Trust’s subsequent recognition as one of the 10 most improved in England reflects the value of that approach.
Some level of post-go-live correction is inevitable in any major implementation. The difficulty arises when it becomes the primary strategy. By that stage, the organisation is already under pressure, with teams adapting to new workflows, performance under scrutiny, and issues that must be resolved within a live operational environment. Corrections take longer, require more effort, and can further disrupt already stretched teams.
The London North West case study shows that recovery is possible, but it also demonstrates the scale of effort required when underlying issues are addressed late, rather than with proactive data due diligence.
What effective transition assurance looks like
A more effective approach begins earlier, with a clear focus on understanding and validating the inherited position before go-live. This includes establishing a reliable baseline of RTT and non-RTT pathways, identifying where data is incomplete or inconsistent, and testing whether workflows and configuration decisions reflect real operational conditions. It also requires the ability to reconcile data quickly during migration and to detect variance early.
MBI’s EPR Transition Assurance model is built around these principles, combining data assurance, operational grip and executive oversight across the full transition period.
In practical terms, trusts should be able to answer a small number of critical questions with confidence:
- Is the waiting list baseline trusted?
- Are pathways complete and consistent before migration?
- Can discrepancies be identified and resolved quickly during transition?
- Do operational processes support control of the PTL after go-live?
- Does the board have clear visibility of pathway risk?
These are operational and governance questions as much as technical ones.
Preventing failure, not correcting it
EPR transitions do not fail solely because of what happens during implementation. In many cases, the conditions for disruption already exist in legacy data and operational processes. A new system will expose those conditions rather than absorb them.
Trusts preparing for transition must prioritise undertaking the necessary data due diligence to validate their inherited position, embed the EPR in operational business rhythms and workflows, re-design reporting suites, train operational staff to use the EPR correctly, and treat pathway assurance as a core component of readiness. This provides a more stable starting point, supports reporting continuity and reduces the need for reactive and extensive post-go-live recovery, which often comes with a significant financial, operational, and administrative burden.
The most effective way to manage remediation is to reduce how much of it is needed in the first place.
Read more about MBI’s EPR Transition Assurance services.





